Foot Conditions
This page will explain in more detail some of the common foot conditions that Foot Health Practitioners can treat. It may be necessary to refer you to a Podiatrist if the condition is outside of My scope of practice or proves to be difficult to resolve.
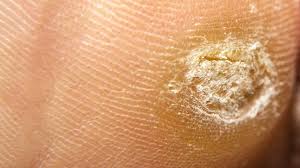
Callus
A callus is an area of hard, thickened skin that develops when the skin is exposed to repeated pressure or friction. It’s the body’s natural way of protecting itself, most often appearing on the heels, balls of the feet, or sides of the toes.
Causes
Footwear that rubs or presses on certain areas.Lo ng periods of walking, standing, or high activity levels. Foot shape issues such as bunions, hammertoes, or flat feet. Uneven pressure when walking. Natural thinning of the skin’s cushioning with age.
Symptoms
Areas of hard, dry, discolourd or rough skin. Discomfort or tenderness when walking or standing. Cracks or splits, especially around the heels. In some cases, especially for people with diabetes or circulation problems, calluses can become more serious if not managed properly.
Corns
A corn is a small, concentrated area of hard, thickened skin that develops due to pressure or friction.
Unlike calluses, corns have a central core that can press into deeper layers of skin, often causing sharp pain or tenderness.
They’re most commonly found on the tops or sides of toes, or on weight-bearing areas of the foot.
Causes
Corns usually form when there is repeated rubbing or pressure against the skin.
Tight or ill-fitting shoes that squeeze the toes. High heels or footwear with narrow toe boxes. Toe deformities such as hammertoes or bunions. Walking pattern that increase friction in certain areas. Thickened or dry skin that doesn’t flex properly.
Symptoms
A small, raised, hard bump (often round and yellowish). Pain or tenderness when pressure is applied. A "stone-in-your-shoe” feeling when walking. Sometimes inflammation or redness around the area. Corns may occur alongside calluses in areas of repeated friction.
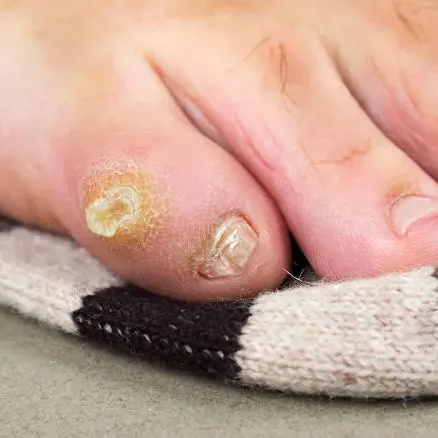
Corn on the little toe
Diabetic Feet
People with diabetes should have their feet checked at least once a year — more often if there are any changes in sensation, circulation, or risk.
Why Its Important
Diabetes can affect the nerves and circulation in your feet — a change known as neurovascular damage.
This can make your feet more vulnerable to injury, infection, and slower healing, often without you noticing early signs.
How often?
NICE recommends that everyone with diabetes has their feet checked at least once a year as part of their routine review.
Those with moderate or high risk changes such as reduced sensation, poor circulation, or foot deformity should be seen more often, from every few months to every few weeks, depending on individual need.
Regular checks help spot small changes early and prevent more serious problems from developing.
Regular checks
Regular foot checks and professional care are important to keep your feet healthy and comfortable.
In many areas, NHS foot health services have become limited, which can mean that people only seek help once a problem has developed.
Prevention
Even simple tasks such as toenail cutting or managing hard skin can become more challenging for people with diabetes, and professional treatment ensures these are done safely and hygienically. Early, preventative care can make a real difference, helping to avoid complications and keep you active and confident on your feet.
Nail conditions
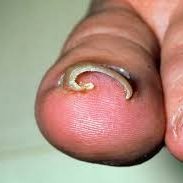
Ingrown Toenails
An ingrown toenail happens when the edge or corner of a nail grows into the surrounding skin.
This can cause the area to become painful, red, swollen, and sometimes infected if left untreated.
It most often affects the big toe, but can occur on any toe.
Causes
Improper nail cutting – trimming nails too short or rounding the corners. Tight or narrow footwear that presses on the toes. Injury or repeated pressure on the toe. Naturally curved nails or inherited nail shape. Thickened nails due to fungal infection or trauma.
Symptoms
Pain or tenderness along one or both sides of the nail. Redness, warmth, or swelling of the surrounding skin. Fluid or pus if infection develops. Difficulty wearing shoes comfortably or walking.
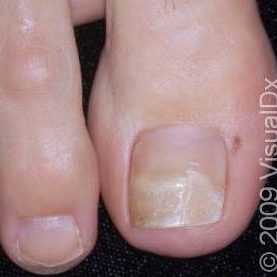
Onycholysis is when the nail separates from the nail bed.
Can be due to trauma or tight fitting shoes, fungal infection or psoriasis
Fungal Nail Infections
A fungal nail infection (also known as onychomycosis) occurs when fungi invade the nail or the skin beneath it.
This can cause the nail to become discoloured, thickened, brittle, or crumbly, or lift away from the nail bed.
Fungal infections can affect one or several nails and are more common on the toenails than the fingernails.
Causes
Fungal nail infections can develop when fungi, often the same type that cause athlete’s foot, enter through small cracks in the nail or surrounding skin.
Most likely to occur if you, have warm, moist feet (e.g., from tight shoes or sweaty socks). Walk barefoot in communal areas such as swimming pools or changing rooms. Have damaged nails or reduced circulation. Live with conditions such as diabetes or weakened immunity
Symptoms
Nails that become yellow, white, or brown. Thickening or crumbly edges. A distorted shape or nail that lifts off the nail bed. Occasionally odour or mild discomfort. May spread to other nails or the skin (e.g., athlete’s foot).
Why Fungal Nails Can Be Hard to Treat
Fungal infections often develop slowly and can be stubborn because the infection lies beneath the hard nail surface. Even with effective treatment, visible improvement can take several months, as healthy nail growth gradually replaces the affected area. Early diagnosis and consistent care greatly increase the chance of success.
A foot health assessment can confirm if the infection is fungal and recommend suitable treatment options. These may include topical or oral antifungal medications, professional nail care to reduce thickness, or newer approaches such as laser therapy. Regular monitoring and good foot hygiene help prevent recurrence and support healthy nail regrowth.